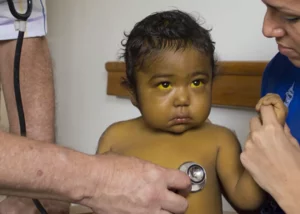
Crohn’s disease presents an inflammation of the digestive system, which starts in the mouth and culminates in the rectum. As for the causes of this condition, they are still unknown, what is known is that it tends to appear when the immune system attacks the organism erroneously.
Some of the factors that directly affect the appearance or increased risk of this disease are genetics, environmental factors, tobacco or cigarette consumption, and the fact that the body usually reacts to the usual bacteria in the intestinal cavity in an abrupt or exaggerated manner.
In addition, this is a disease that can occur at any point in life, however, it is more likely to occur between the ages of 15 and 35.
Inflamed liver and Crohn’s disease
Crohn’s disease, or inflammatory bowel disease (IBD), can migrate to organs other than the digestive system. Among them are the liver, bile ducts and gall bladder. On this subject it is highlighted that hepatobiliary manifestations are more common than the rest, some of these are:
- 1. Cholelithiasis or stones in the gallbladder: it is known that between 13-24% of patients with Crohn’s disease may present cholelithiasis.
- 2. Fatty liver: in many other diseases the fat present in the liver is a disadvantage or risk factor, in the case of IBD the same thing happens, so fatty liver disease can develop.
- 3. Primary sclerosing cholangitis: it is a chronic and progressive inflammation of the bile ducts. The bile ducts are used to transport bile from the liver, where it is formed, to the intestine, where it will help digest food, previously stored in the gallbladder. (Educainflammatory pathway).
Of all the conditions, this is the least frequent to appear in patients with IBD, in fact, most of the time the evolution of this is independent of Crohn’s disease.
- 4. Hepatic alterations produced by medications: the use of different drugs for the treatment of Crohn’s disease will be very useful, however, they have side effects that can generate toxic hepatitis.
Chronic hepatitis and IBD
Patients who have hepatitis B or who have had it can reactivate the disease after taking immunosuppressants. Faced with this possibility, it is common to recommend or prescribe antivirals, so that this risk is significantly reduced. As for hepatitis C, it is likely that it is necessary to treat the condition before taking immunosuppressants.