Hepatic encephalopathy is a serious complication that can affect people with liver disease. In this article, we will explore what hepatic encephalopathy is, its stages, how it is classified and whether there is treatment. Read on to learn more about this topic!
What is hepatic encephalopathy?
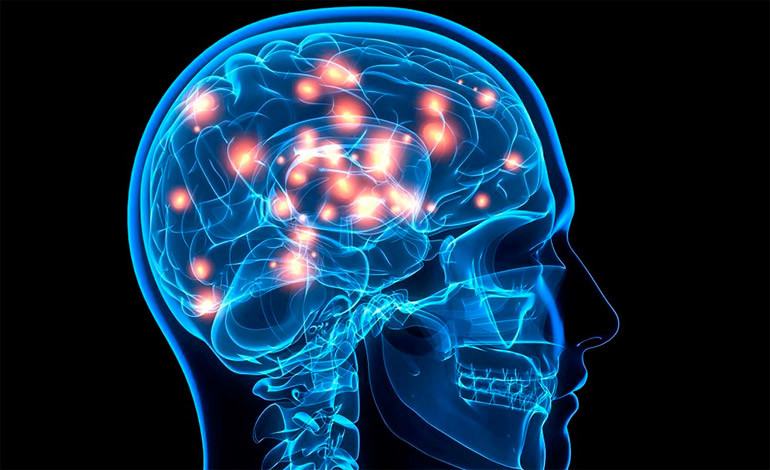
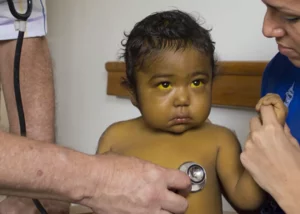
Hepatic encephalopathy is a brain dysfunction that occurs as a result of a buildup of toxins in the body due to liver malfunction. When the liver cannot properly eliminate toxic substances, such as ammonia, they accumulate in the blood and adversely affect the brain. As a result, people can experience a wide range of neuropsychiatric symptoms, ranging from subtle personality changes to mental confusion and, in severe cases, coma.
What are its stages?
Hepatic encephalopathy is classified into different grades according to the severity of symptoms. Grades range from mildly altered mental status to deep coma. As the disease progresses, symptoms may worsen and significantly affect the quality of life of the affected person.
- Grade 0: no evident neurological alterations are observed in the patient. Mental status and brain function are normal. There are no clinically detectable symptoms of hepatic encephalopathy.
- Grade 1: mild and subtle symptoms of hepatic encephalopathy may appear. The patient may experience mild impairment of mental status, such as subtle personality changes and decreased attention span. Sleep disturbances, such as insomnia or daytime sleepiness, may also occur. The level of consciousness may fluctuate slightly.
- Grade 2: symptoms become more evident. The patient may exhibit temporal and spatial disorientation, memory difficulties and behavioral changes. More pronounced sleep disturbances, such as a reversed sleep-wake pattern, may also appear. In addition, tremors in the extremities may be observed, and the level of consciousness may fluctuate significantly.
- Grade 3: the deterioration of mental status is more pronounced. The patient may experience significant confusion, disorientation in time and space, language and problem solving difficulties. Sleep disturbances may be more severe, with periods of insomnia and intense drowsiness. Involuntary movements, such as tremors or muscle twitching, and abnormal reflexes may also occur. The level of consciousness may fluctuate between drowsiness and alertness. Seizures may be present in this grade.
- Grade 4: this is the most severe stage of hepatic encephalopathy. The patient may be comatose or in a deep stupor, with an almost total loss of response to external stimuli. Muscle rigidity, involuntary twitching and myoclonus (sudden rapid movements of the muscles) may be present. Respiratory function may be compromised, and intensive medical attention is required to prevent life-threatening complications.
How is hepatic encephalopathy classified?
Hepatic encephalopathy is classified into different stages according to symptoms and brain function. The most commonly used classification is the West Haven scale, which ranges from grade 0 to grade 4. Grade 0 refers to the absence of symptoms, while grade 4 indicates a deep coma.
Is there treatment?
Fortunately, there are treatment options available for hepatic encephalopathy. The main goal of treatment is to reduce the accumulation of toxins in the body and improve brain function. Therapeutic approaches include dietary changes, medications to reduce ammonia production in the intestine, antibiotics to reduce ammonia-producing bacteria and, in severe cases, the possibility of liver transplantation.
It should be emphasized that hepatic encephalopathy can be caused by other liver diseases such as cirrhosis. While it is true that the best thing you can do to cure a condition is to see a professional, it is even better to prevent such disease. Following a balanced diet, exercising, not overindulging in alcohol, and in short, not straining the liver, can prevent these debilitating conditions from ever occurring in the first place, or at least significantly reduce your risk. Encephalopathy can be successfully prevented from falling into a coma and needing a liver transplant, which can be traumatic not only for the person affected, but also for those around them.

It is important to note that the treatment of hepatic encephalopathy should be individualized and tailored to the specific needs of each patient. Therefore, it is essential to seek specialized medical care and follow the indications of the team of health professionals.
In summary, hepatic encephalopathy is a severe complication of liver disease that affects brain function due to the accumulation of toxins in the body. With varying stages of severity and classifications, it is critical to seek appropriate treatment to manage symptoms and improve quality of life. If you or someone you know is experiencing symptoms of hepatic encephalopathy, we recommend consulting a medical specialist for an accurate diagnosis and appropriate treatment.