Liver fibrosis is a condition that affects the liver, leading to the development of scar tissue. In this article, we will explore all about it, its symptoms, and the different stages of this liver disease. Additionally, we will discuss various treatment options available.
What is Liver Fibrosis?
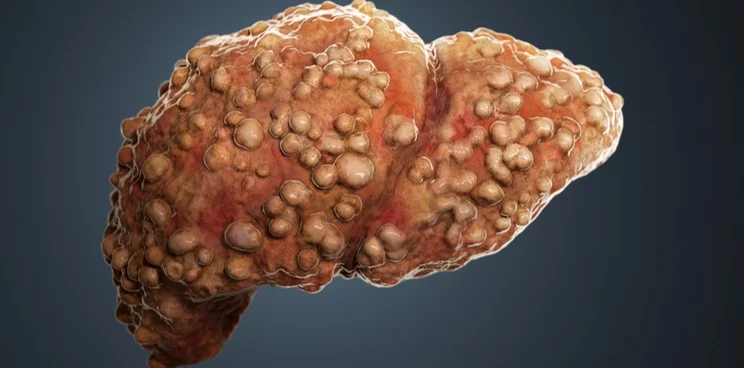
Liver fibrosis is a progressive condition characterized by the accumulation of excessive scar tissue in the liver. It occurs as a response to liver damage or inflammation, such as that caused by chronic viral hepatitis, alcohol abuse, or non-alcoholic fatty liver disease (NAFLD). As it advances, it can impair liver function and ultimately lead to cirrhosis if left untreated.
What are the Symptoms?
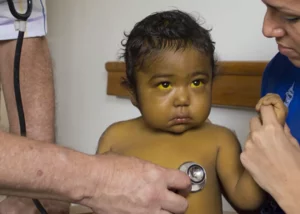
Liver fibrosis often progresses silently, with no noticeable symptoms in the early stages. However, as the condition worsens, some individuals may experience symptoms such as fatigue, abdominal discomfort, unexplained weight loss, jaundice (yellowing of the skin and eyes), and swelling in the legs and abdomen. It’s important to note that symptoms can vary depending on the underlying cause.
What Stage of Liver Disease is Fibrosis?
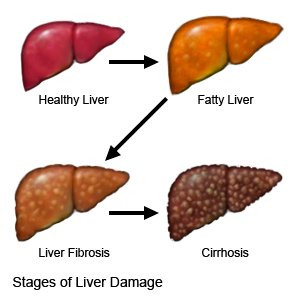
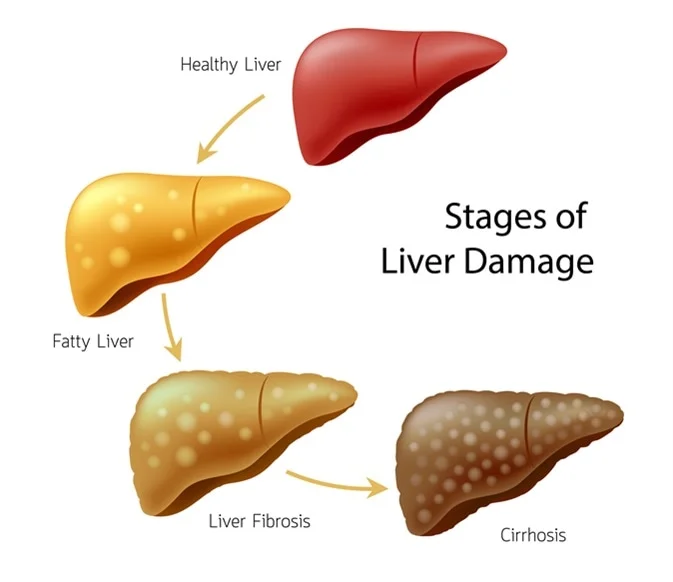
Liver fibrosis is classified into stages to assess the extent of liver damage and guide appropriate treatment decisions. The staging systems provide a standardized way of categorizing the severity of the disease and determining the prognosis for individuals with liver disease. One widely used staging system is the METAVIR scoring system, which ranges from F0 to F4.
- Stage F0 indicates no fibrosis, meaning there is no significant scarring or fibrosis present in the liver. At this stage, the liver tissue is relatively healthy, and the liver functions normally.
- Stage F1 represents minimal fibrosis, where there is mild scarring in the liver, but it has not yet caused any significant impairment of liver function. Fibrosis at this stage is generally reversible with appropriate treatment and lifestyle changes.
- Stage F2, it indicates moderate fibrosis. At this point, the scarring in the liver becomes more pronounced, indicating a progression of liver disease. It is crucial to intervene at this stage to prevent further fibrosis and subsequent complications.
- Stage F3 corresponds to advanced fibrosis. The liver has developed extensive scarring, and liver function may start to be noticeably impaired. Individuals at this stage are at a higher risk of developing cirrhosis if the underlying cause is not effectively managed.
- Stage F4 signifies cirrhosis, the most severe stage of liver fibrosis. Cirrhosis is characterized by widespread and irreversible scarring of the liver tissue, leading to significant liver dysfunction.
At this stage, liver function is severely compromised, affecting its ability to perform vital functions such as detoxification, metabolism, and blood clotting. Individuals with cirrhosis are at an increased risk of developing complications like portal hypertension, ascites (fluid accumulation in the abdomen), hepatic encephalopathy, and liver cancer.
Treatment Options:
Treatment options for liver fibrosis aim to prevent further progression of the condition, manage underlying causes, and reduce the risk of complications. The specific treatment approach may vary depending on the underlying cause of liver fibrosis. Here are some common treatment options:
- Lifestyle Modifications: Adopting a healthy lifestyle is crucial in managing liver fibrosis. This includes:
- Maintaining a Balanced Diet: consuming a diet rich in fruits, vegetables, whole grains, lean proteins, and healthy fats while limiting the intake of processed foods, saturated fats, and added sugars.
- Alcohol Abstinence: completely avoiding alcohol consumption is essential, as alcohol can worsen liver damage and accelerate fibrosis progression.
- Regular Exercise: engaging in regular physical activity can help improve overall liver health and reduce the risk of complications associated with liver fibrosis.
- Weight Management: maintaining a healthy weight and managing conditions such as obesity and diabetes can help alleviate stress on the liver and reduce fibrosis progression.
- Medications: Depending on the underlying cause of liver fibrosis, specific medications may be prescribed. These can include:
- Antiviral Medications: if liver fibrosis is caused by chronic viral hepatitis (such as hepatitis B or C), antiviral drugs may be prescribed to suppress viral replication and reduce inflammation in the liver.
- Medications for Autoimmune Conditions: in cases where autoimmune conditions contribute to liver fibrosis, medications that suppress the immune system, such as corticosteroids or immunosuppressants, may be prescribed to reduce liver inflammation.
- Medications for Non-Alcoholic Fatty Liver Disease (NAFLD): lifestyle modifications, weight loss, and certain medications may be recommended to manage liver fibrosis associated with NAFLD. These medications may help reduce liver inflammation, insulin resistance, and fat accumulation in the liver.
Other treatment options
- Management of Underlying Conditions: Treating and managing underlying conditions that contribute to liver fibrosis is essential. For example:
- Control of Diabetes: proper management of diabetes through medication, diet, and lifestyle changes can help minimize progression.
- Weight Loss: in cases where obesity is a contributing factor, weight loss through a combination of diet and exercise can help reduce liver fat.
- Liver Transplantation: in severe cases where liver function is significantly impaired, and complications arise, liver transplantation may be considered.
A liver transplant involves replacing the diseased liver with a healthy liver from a deceased or living donor. This option is typically reserved for individuals with advanced cirrhosis or liver failure.
Conclusion:
Liver fibrosis is a progressive condition characterized by the buildup of scar tissue in the liver. While it may initially have no noticeable symptoms, its progression can lead to significant liver damage and cirrhosis.
Understanding the stages of this liver disease is crucial for early detection and timely intervention. By adopting a healthy lifestyle, following prescribed medication and considering transplantation when necessary, people with this disease can better manage the disease and improve their overall quality of life.