When liver diseases reach a point of being life-threatening, a liver transplant becomes a hope of salvation for that patient. In this article, we will explain when it is necessary to perform a liver transplant, the reasons behind this intervention, its implications and risks. If you want to know more about this topic, continue reading!
When is it necessary to perform a liver transplant?
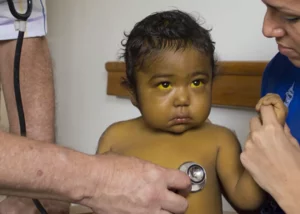
Is necessary when the original organ is so damaged that it cannot fulfill its vital functions. Severe liver diseases, such as cirrhosis, chronic hepatitis, liver cancer, and inherited metabolic diseases, can lead to this critical situation. Determining the need for a transplant is based on a number of factors, such as: the patient’s general health, the degree of liver damage, and the response to previous medical treatments.
Reasons why a liver transplant is performed
1.- Advanced cirrhosis: generally caused by chronic alcoholism or chronic hepatitis infection, which gradually damages the liver tissue until reaching an advanced stage where the liver cannot function properly, considerably deteriorating the patient’s quality of life.
2.- Liver cancer: in the case of advanced stage, a transplant may be the only curative option. However, not all patients with liver cancer are candidates for a transplant, as they must meet other sets of conditions.
3.- Hereditary metabolic diseases: such as Wilson’s disease or glycogen storage disease, they can lead to a serious deterioration in the functionality of the liver. In these cases, a liver transplant may be necessary to improve quality of life and prolong survival.
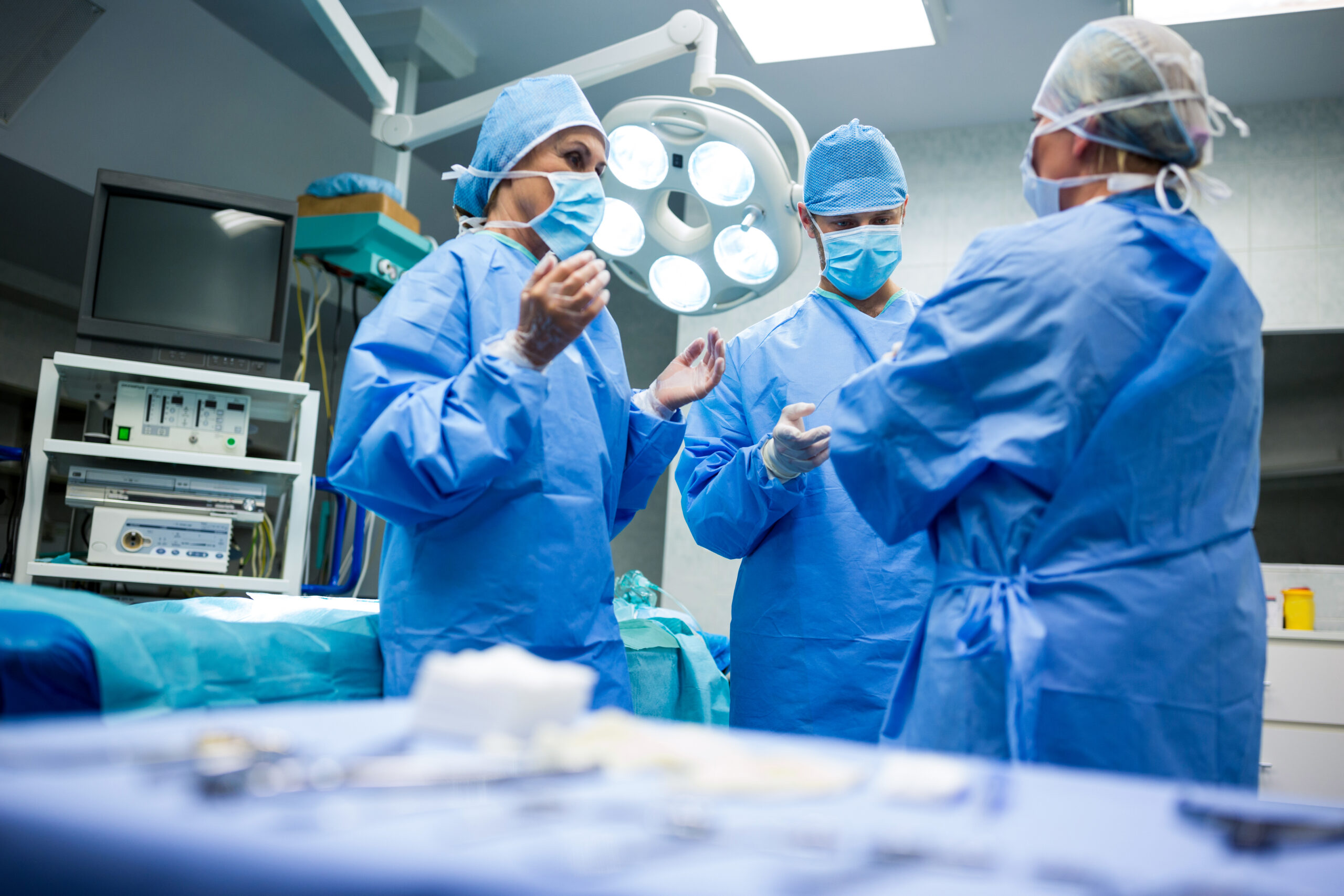
What does the surgery involve?
Liver transplant is a high-level surgery in which the damaged liver is replaced with a healthy one from a compatible donor (it can be a portion of healthy liver). Before surgery, the patient is thoroughly evaluated to determine its suitability. Next, a donor is sought, which may be a living donor or a deceased donor, depending on the situation.
After surgery, the patient will require intensive care and close monitoring to prevent rejection of the transplanted organ and apply the treatment indicated by the treating physician and manage any complications.
What are your risks?
While liver transplant can save lives, it is not without risks. The main ones are:
- Organ rejection: the patient’s immune system may recognize the new liver as an invader and try to destroy it. This is controlled with immunosuppressive medications, but can still be a challenge to overcome.
- Infections: after surgery, patients are more susceptible to infections due to suppression or vulnerability of the immune system.
- Surgical complications: as with any surgery, there are inherent risks associated with the operation itself, such as bleeding or problems with wound healing.
In conclusion, liver transplant is a vital option for those patients whose lives are threatened by serious liver diseases. Careful assessment, selection of appropriate donors, and risk management are critical to the success of this intervention. Despite the challenges, liver transplantation offers a second chance and hope for a healthier life for those who desperately need it.